I still smell the red earth of Kitale when Nairobi traffic roars.
It’s 2018. I’m 22, clutching a nursing diploma from a small college in Western Kenya, boarding a matatu bound for the city. My mother stands at the shamba gate, her callused hands wrapped around a hoe. “Go heal the world, Ann,” she says. “But don’t forget the soil.”
I thought I understood what she meant. I didn’t. The city would teach me how to read monitors, operate ventilators, and move with clinical precision through air-conditioned wards. But it would also teach me something else: how success can quietly unroot you.
The Migration Written in My Bones
Kenya’s health worker exodus is often told in numbers. By 2026, nearly 70% of medical resources are concentrated in urban centers like Nairobi. Universal Health Coverage (UHC), launched in 2023 with promises of equity, was meant to close that gap. But on the ground, the divide is widening.
Rural maternal deaths rose by an estimated 12% last year, according to Ministry of Health data. In cities, private hospitals expand, upgrade, and profit. Clinics in villages often stall, remain understaffed, lack equipment, and receive little attention. For me, the issue isn’t policy. It’s personal. It’s the distance between where I come from and where I now work.
Where Care Begins With Calluses
In Trans-Nzoia, care didn’t look like machines. It looked like effort. When my brother had malaria, my mother crushed herbs into poultices and prayed through the night. The nearest dispensary was a tin-roofed structure with one nurse called Esther, who cycled nearly 20 kilometers each day to reach it.
“We ration paracetamol like gold,” she once told me, laughing without humor. I began shadowing her at sixteen. She worked with instinct, memory, and resilience. No machines, no backup. Just her hands. Back then, I wanted to be her.
But by the time I graduated, the path ahead had shifted. Kenya’s youth population, 65% under 35 years, was pushing outward toward cities and toward opportunity. A private hospital in Nairobi could offer three times what a rural posting paid. So I left, but Esther stayed.
Last month, I called her. “We lost three mothers this week,” she said. “No oxygen. No staff. UHC cards? They don’t help us here.” At home, the fracture is quieter but just as real.
My sister Jane now farms our two acres. “You send money,” she tells me, “but who treats the sick?”
My cousin Peter, an unemployed engineer, puts it more bluntly: “The city swallows dreams. Then it spits out what’s left.”
Each year, roughly 2,000 nurses leave rural postings for urban jobs. It’s not just migration; it’s redistribution. Skills move. Systems weaken.
The Seduction of the City
My first shift in a private hospital in Nairobi felt like stepping into another country. Marble floors. Soft lighting. Machines that beeped in steady rhythms. Everything worked. I assisted in intubating a CEO’s son. The ventilator hummed beside him, just precise, dependable, and expensive. It was the kind of care I had never seen growing up.
My salary tripled within months. I sent money home. I bought my mother a solar lantern. By every measure, I was succeeding. But success in the city comes with rules.
In public hospitals, a nurse may handle up to 50 patients at once. In private facilities, the ratio drops to about five. The difference isn’t just workload but about attention, dignity, and survival. And then there’s the unspoken rule: care follows money. “We triage by wallet,” a colleague once joked. It wasn’t really a joke.
Audits of UHC implementation show urban coverage nearing 85%, while rural regions lag far behind. Access isn’t equal; it’s stratified. First, I began to feel it in smaller ways. The patients we admitted. The ones we didn’t.
A woman from a rural area arrived one night in critical condition. There were no beds. “She’s malnourished,” I wrote in her chart, reducing her life to a line of clinical shorthand. She reminded me of home.
Climbing Up, Drifting Away
Somewhere along the way, my life began to change faster than I could track. I started dating a doctor. My evenings shifted from village phone calls to rooftop dinners. My language changed. My expectations changed. But the distance from home wasn’t just physical anymore. It was internal.
In 2025, more than 10,000 nurses participated in strikes demanding better pay and conditions. I didn’t join them. I stayed in the private system, where the pay was steady and the workload manageable.
I told myself I had earned it. But burnout doesn’t always come from overwork. Sometimes it comes from a contradiction, living in two realities that refuse to reconcile.
Two Systems, One Country
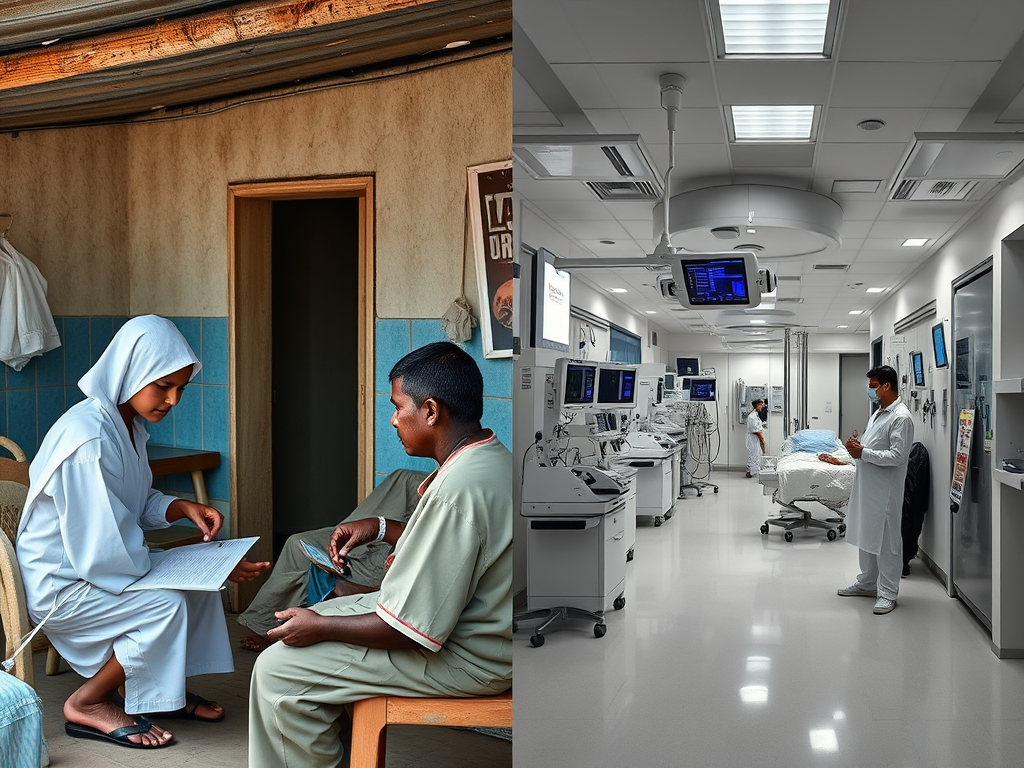
The gap between rural and urban healthcare isn’t abstract. It’s structural.
- In rural areas, a single nurse may serve up to 100 patients.
- In private urban hospitals, that number can drop to five.
- Rural clinics rely on basic tools; urban facilities operate with advanced imaging, ICU units, and continuous monitoring.
- Salaries differ drastically, shaping not just livelihoods but decisions: who stays, who leaves, and who returns.
I send money home every month. It helps. It matters. But it doesn’t replace presence. And it doesn’t rebuild systems.
The Breaking Point
In early 2026, floods hit Trans-Nzoia. My mother called me late at night. My sister had gone into early labor. “There’s no incubator,” she said. “No doctor.”
I left Nairobi at dawn, pushing through traffic, then distance, then memory. By the time I arrived, the power was out. We worked under lantern light. No monitors. No machines. Just hands. My hands.
For the first time in years, I felt unsure, not because I didn’t know what to do, but because I had forgotten how to do it without support. City training had made me precise. Rural reality demanded improvisation. The baby survived. But something in me shifted.
What It Costs to Leave
Kenya’s healthcare migration tells a familiar story: individuals rise and systems strain. We move toward opportunity, stability, and better lives. But every movement leaves something behind.
UHC was meant to balance these factors, to make care universal, not geographic. But implementation is uneven, and time is running against political timelines. In rural areas, frustration is growing. Protests are beginning to surface. The promise of equity feels distant.
I find myself in a difficult position. My salary built my mother a better house. It pays school fees. It keeps the farm running. But it didn’t keep me there.
Learning to Return
Now, I split my time. Part of me still works in Nairobi, in clean wards filled with quiet machines. The other part travels back, volunteering in rural clinics, relearning what I once knew instinctively. It’s not a solution. It’s a compromise. But it’s a start. Because what I’ve come to understand is this: healthcare isn’t just about infrastructure or policy. It’s about presence. And presence cannot be centralized.
The Soil Remembers
When I think back to that morning in 2018, I understand my mother differently now.
“Don’t forget the soil,” she said. She wasn’t warning me about leaving. She was warning me about disconnecting. I became so adapted to one system that I could no longer function in another. About mistaking personal progress for collective progress.
I left the village to heal others. But somewhere along the way, I stopped seeing what needed healing most. Not just patients. But the gap between where we go and what we leave behind.






Leave a comment