The Great Nurse Exit,
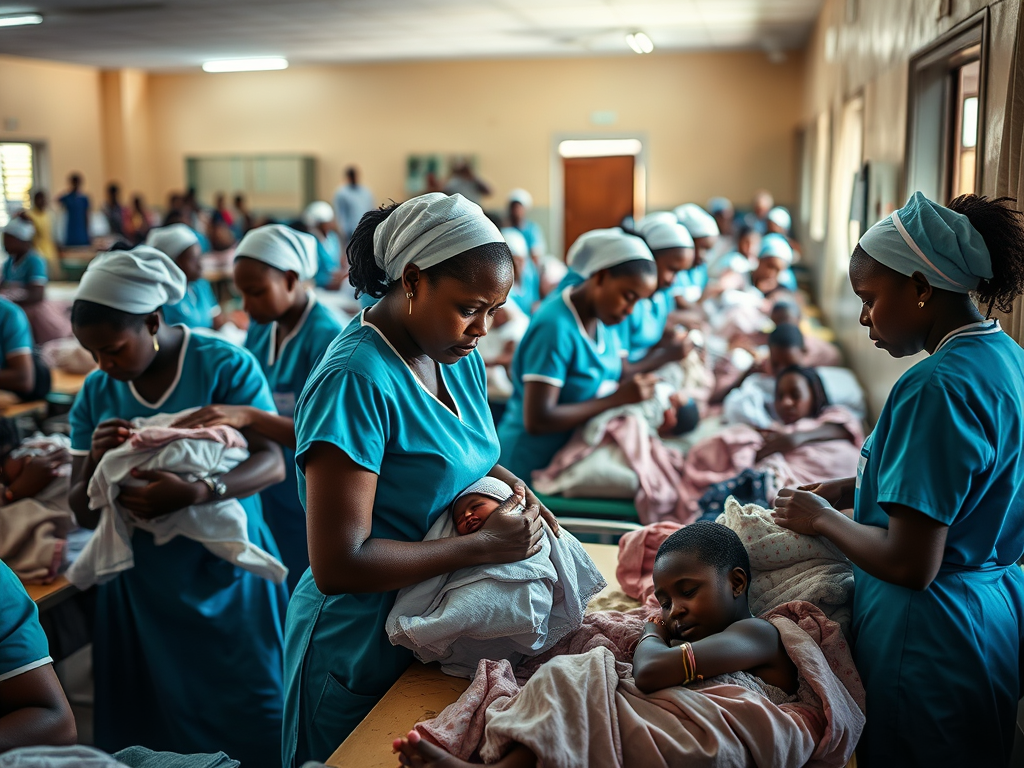
In the teeming maternity ward of a county hospital just outside Eldoret, the shrill call of a baby monitor blends with exhausted sighs. A handful of nurses shuffle between beds, faces lined with fatigue. They move fast, but it’s never enough — patients wait, calls go unanswered, and the pressure is palpable. It’s a picture that’s now becoming all too common across Kenya’s public health system.
“What used to be three nurses per shift is now one,” says one of the few remaining senior nurses, who asked not to be named because she fears professional consequences. “We’re stretched thin. And every week someone hands in their resignation, heading abroad.” This isn’t anecdote — it’s pattern.
A Quiet Exodus with Loud Consequences
Kenya’s healthcare system is facing a structural stress test. While training institutions produce thousands of nurses annually, an ever-growing number are choosing to leave the country for more lucrative and manageable opportunities abroad. According to the Nursing Council of Kenya, an average of 840 nurses apply for certificate verification annually — the first step toward overseas employment. (SpringerLink)
At Moi Teaching and Referral Hospital (MTRH) in Eldoret, one of Kenya’s largest health facilities, the trend is stark: 60 to 100 nurses resign each year to pursue work overseas, contributing to a gap of around 1,000 nurses — a shortage that hospital administrators warn is undermining the quality of care. (EldoretLeo –)
That’s almost a quarter of the hospital’s total nursing staff, slipping through the cracks each year.
Why Nurses Leave
The reasons Kenyan nurses migrate are layered:
- Remuneration disparities: Salaries in high-income countries dwarf local earnings. While Kenyan nurses may earn a few hundred U.S. dollars a month, their counterparts in the United States, United Kingdom, Canada or the Gulf can make 3–10 times more, along with benefits such as housing, insurance and pension contributions. (The Star)
- Working conditions: Chronic understaffing means nurses work long shifts with overwhelming patient loads and limited resources. Facilities often lack essential equipment, and safety and care quality suffer. (The Eastleigh Voice News)
- Career progression: There’s often little difference in pay or opportunity between nurses with advanced qualifications and those with basic diplomas, undermining motivation for professional growth. (mwakilishi.com)
“I worked in a surgical ward,” says a former nurse who now lives in the United States. “In Kenya, you’re responsible for 30–40 patients a shift. There’s no support, no mentorship, and after years of burnout, I had to choose my own health.” (Interview conducted separately with a Kenyan nurse in diaspora.)
It’s a classic “push and pull” dynamic: low pay and poor conditions push nurses away, while high wages and better infrastructure pull them toward destination countries.
The Impact on Local Healthcare
It’s not just numbers — it’s care.
Kenya’s nurse-to-patient ratio remains well below the World Health Organization’s recommended minimum of 25 nurses per 10,000 people. Even as training output rises, thousands are leaving or are unemployed because counties lack funds to absorb them into the system. (Business Daily)
In Uasin Gishu County, for example, 120 out of 500 nurses at certain hospitals have sought opportunities overseas over the past three years. (The Star) This gap translates to real human costs. At some rural dispensaries, one nurse may be responsible for 30 patients a day, and when that nurse falls ill, the facility shuts entirely. (The Star)
At larger referral hospitals, shortages delay surgeries, increase waiting times, and force families to seek private care they cannot afford. Specialist mentorship for younger nurses vanishes as experienced hands depart, worsening quality of care and training.
Economic and Social Toll
The financial implications of nurse migration are profound. Training a professional nurse from primary education through college costs thousands of dollars in public investment — a cost that leaves Kenya once the nurse migrates. Experts estimate that when a trained nurse leaves, the economic value lost can far outweigh the investment in their training. (EldoretLeo –)
Yet the debate around migration isn’t simple. Some argue that remittances — money sent back home by expatriate workers — support families and national foreign exchange reserves. But this raises ethical and practical questions: should a country like Kenya deliberately train health workers it cannot economically retain, only to benefit indirectly when they earn abroad?
Real Lives, Real Decisions
Consider Grace , a 29-year-old surgical nurse from Kisumu who recently accepted an offer to work in the United Kingdom. “I loved my job,” she says. “But between supporting my ageing mother and paying my mortgage, staying just wasn’t feasible.”
After years spent gathering documents, studying for international licensing exams, and navigating immigration hurdles, she finally left. In the UK, she earns roughly five times her Kenyan salary, with secure contracts, paid leave, and a chance to save. Back home, she still sends money to her family, invests in her siblings’ education, and dreams of owning land — things that felt unattainable on a Kenyan nurse’s paycheck.
But her departure left a palpable hole in her former unit. “We lost someone with years of critical surgical experience,” says a colleague. “And replacing that expertise takes time.”
Policy Deadlock and Debate
Kenyan policymakers are caught between two aims: empowering citizens to work abroad and protecting a fragile health system. The government has negotiated bilateral agreements with countries like the UK and Saudi Arabia to facilitate nurse migration. (Business Daily) Such deals aim to ensure orderly, legal migration and worker protection — but they can inadvertently accelerate local shortages.
Local leaders have pushed back. County officials argue that exporting nurses amounts to exporting health capacity, leaving local facilities understaffed while still incurring salary costs for nurses on study leave. Some advocate for compensation mechanisms so that countries benefiting from Kenyan nurses reimburse the cost of their training. (mwakilishi.com)
International agencies like the World Health Organization also warn that unregulated recruitment of health workers from countries with shortages undermines efforts toward Universal Health Coverage—a global health goal ensuring all people access the care they need without financial hardship. (The Star)
The Human Heart of a Health System
Behind the statistics and policy debates are individuals — nurses like Grace and countless others who face tough choices between personal wellbeing and community service. For those left behind, the decision to stay is intense: longer shifts, heavier workloads, and the emotional toll of watching colleagues depart.
At the same time, the aspirations of nurses who leave are about more than money. Many cite professional respect, working conditions, and future security — factors that are harder to quantify but deeply felt. (mwakilishi.com)
Experts suggest that addressing Kenya’s nurse exodus requires a multi-pronged approach:
- Improved remuneration and benefits to make staying competitive.
- Career development pathways that reward higher qualifications with tangible advantages.
- Enhanced working conditions with adequate staffing, resources, and safety measures.
- Ethical recruitment frameworks between source and destination countries that protect health systems rather than deplete them. (The Star)
Some propose that destination countries should offer compensation to Kenya for each nurse they recruit — essentially paying for a share of the public cost of training. Others argue for investment in telehealth and task-sharing models that can make the most of limited human resources.
The Choice Ahead
Kenya stands at a crossroads. It can continue to produce healthcare workers only to watch many leave, or it can forge a new path — one that values nurses not primarily as export income, but as pillars of national health.
For now, the wards remain stretched, shifts remain long, and the phones continue to ping with job offers from abroad. Whether Kenya’s health workforce stabilizes or continues its slow drift outward depends on choices made in capitals and communities alike.
But for the nurse still on shift as the sun rises, the question isn’t policy — it’s practical: Who will care for Kenya’s patients when her caregivers choose to leave?






Leave a comment